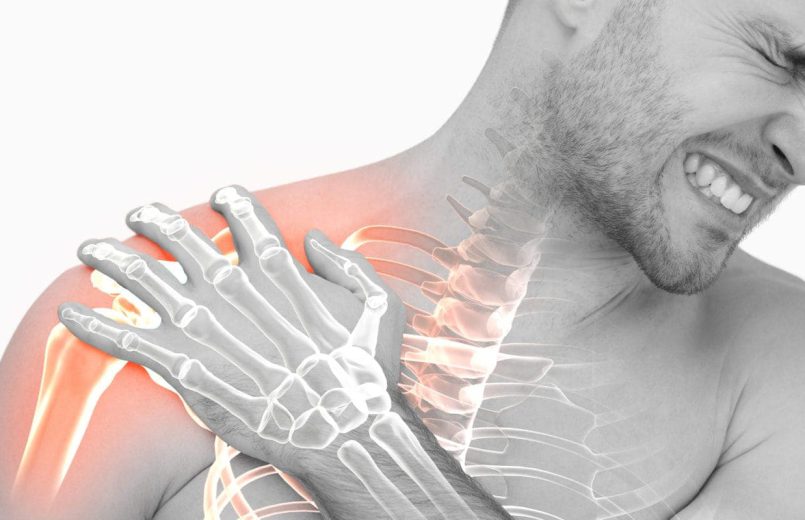
Maybe you have never heard this expression. And is that this disorder is not as well known as osteoarthritis or tendinitis but it is quite frequent, especially in women. Do you feel pain and stiffness? Attentive, because maybe it’s your case.
Physiotherapist in Dwarka calculates that between 3 and 5% of the population will suffer the so-called “frozen shoulder” at some point in their life. Although initially, this percentage may seem low, it increases considerably among certain groups.
80-90% of cases occur in women between 40 and 70 years, especially after menopause (from 50). But they are not the only ones affected. We tell you what this pathology consists of, how to identify its symptoms, which people are more at risk of suffering it, and what treatments exist to overcome it.
WHAT IS THE FROZEN SHOULDER”?
The medical term is adhesive or retractable capsulitis, although the same specialists use the expression “frozen shoulder” because it is much more graphic and easy to understand.
This disorder begins causing a very intense pain in the shoulder that usually gets worse at night. This usually starts suddenly and without a cause that justifies it (bad gesture, injury, etc.).
After a while, the person who suffers begin to notice a stiffness in the joint that ends up in the difficulty or inability to move the shoulder normally. Hence, the term “frozen shoulder.”
The immobility increases progressively until the person is unable to perform such habitual gestures as raising the arm and passing the hand over the head or carrying it towards the back too, for example, fastening the bra, knotting the apron or scratching.
This disorder occurs when there is inflammation in the capsule of the joint, which hinders the mobility of the ligaments that unite the bones that make up the shoulder. However, the cause that causes this inflammation is still unknown.
WHEN THERE IS MORE RISK OF WHICH HAPPENS
Although the reason is not known either, it is demonstrated that certain people are more at risk of suffering from “frozen shoulder”. And is that this disorder is associated with the following factors or pathologies:
- Hormonal changes. The majority of cases occur in women over 40 years, and especially after menopause.
- Diabetes. People who suffer from this disease also have a higher risk of suffering from “frozen shoulder”.
- Thyroid problems Whether you suffer from hypothyroidism or hyperthyroidism.
- Heart surgery. People who have cardiovascular problems and have undergone open-heart surgery are also among the risk groups.
- Shoulder injuries Having fractures, surgery on this joint and its immobilization for a while may favor adhesive capsulitis.
If you are in one of these risk groups, you should be alert to the first symptoms, since early diagnosis can help to make the recovery more favorable.
In addition, people with diabetes or with thyroid problems can reduce the risk of suffering “frozen shoulder” if they maintain good control of their disease.
THE TREATMENT DEPENDS ON THE MOMENT
Although in most cases recovery of shoulder mobility is total, the process is very slow and frozen shoulder treatment in Dwarka can last between 6 months and 2 years.
Although sometimes the “frozen shoulder” heals itself after 18-24 months, without treatment and spontaneously, it is advisable to go to the best physiotherapist in Dwarka as soon as possible since the treatment can advance the process, alleviate the symptoms and prevent mobility is reduced.
The physiotherapy doctor in Dwarka will assess the most appropriate treatment according to the phase of the disorder in which the patient is:
- Inflammatory phase. The pain is very intense, especially at night, which makes it difficult to rest. But there are still no mobility problems. At this stage, the best physiotherapy doctor in Dwarka usually prescribes analgesics and anti-inflammatories and advises avoiding those movements that may increase pain. Generally, it is advisable to combine a certain rest with gentle stretching exercises. In those acute cases in which the pain does not decrease, it may be necessary to perform some infiltration of steroids (corticosteroids) in the joint.
- Freezing phase. The shoulder begins to show rigidity and mobility problems are increasing, although the pain usually decreases. At this stage, physiotherapy in Dwarka is fundamental, although perseverance is needed. The number of rehabilitation sessions per week will depend on each case, but they can be daily and for several months. Recovery exercises should always be performed by a specialist physiotherapist in Janakpuri, who will also teach the affected person how to perform the stretching exercises correctly at home.
- Recovery or defrosting phase. Mobility progressively improves, although it may be necessary to continue doing exercises for a total recovery and to prevent future relapse.
Most people suffering from “frozen shoulder” respond well to this treatment, as long as they are constant both when going to physiotherapy sessions and when performing the exercises indicated at home.
However, in those cases in which a clear improvement is not achieved, it may be necessary to perform surgery. Normally the operation is performed by arthroscopy in Delhi, through small incisions, and with local anesthesia, and the objective is to “free” the ligaments to restore mobility to the shoulder joint.
DISCARD OTHER PROBLEMS
The shoulder is one of the joints with greater mobility and, therefore, one of the most prone to pain. Therefore, when it does not return in several days it is necessary to go to the orthopaedic in Delhi to make a diagnosis.
In addition to adhesive or retractable capsulitis (“frozen shoulder”), these are the most common problems that can cause pain in this part of the body:
- Contractures The muscles of the shoulder or cervical muscles contract due to a bad gesture, a bad posture repeated or sustained in time or tension.
- Calcifications They consist of the accumulation of calcium in the supraspinatus tendon, usually due to minor trauma, tears or inflammation. It usually affects people between 30 and 50 years old.
- Arthrosis This degenerative disease, in which a loss of cartilage occurs, can also affect the shoulder, as well as other joints such as the knee. In addition to pain and limited mobility, crunches (crepitations) may be felt when moving.
- Rotator cuff injuries. It is formed by muscles and tendons that provide stability to the bones of the joint and facilitate movement. The tearing or breaking of these tissues by some trauma, sudden movement or wear are some of the most common problems, as well as the inflammation of some tendon (tendonitis).
The symptom of something more serious. When the pain does not vary with the movement, it can be a symptom of some disease that has nothing to do with the shoulder, such as a heart problem (in this case, it is usually accompanied by a feeling of tightness in the chest) or a pulmonary pathology, for example of the pleura. Some types of lung cancer can cause shoulder pain, especially when the tumor is large and press on the area near the joint.